Top 8 Tips to Optimize Your Blood Sugar Level by Dr. Joseph Mercola for Mercola
Insulin is essential to staying alive; unfortunately, the vast majority of people have resistance to this essential hormone, speeding up the aging process and contributing to the development of degenerative diseases. Any meal high in grain and sugar carbs typically generates a rapid rise in blood glucose.
To compensate, your pancreas secretes more insulin into your bloodstream to lower your blood sugar. Insulin, however, is also very efficient at lowering blood sugar by turning it into fat. The more you secrete, the more fat your body will accumulate.
If you consistently consume a high-sugar, high-grain diet, your blood glucose level will be correspondingly high and over time your body becomes desensitized to insulin, requiring more and more of it to get the job done. Eventually, you become insulin resistant and prone to weight gain, and then full-blown diabetic.
Prediabetes1 is defined as an elevation in fasting blood glucose between 100 milligrams per deciliter (mg/dl) and 125 mg/dl. At 126 mg/dl on two separate occasions, it formally becomes Type 2 diabetes. According to the U.S. Centers for Disease Control and Prevention, an estimated 84.1 million American adults — about 1 in 3 — are prediabetic,2,3 and most are unaware of this fact.
However, any fasting blood sugar regularly over 90 in my book suggests insulin resistance, and findings by the late Dr. Joseph Kraft — former chairman of the department of clinical pathology and nuclear medicine at Presence Saint Joseph’s Hospital, Chicago, and author of “Diabetes Epidemic and You: Should Everyone Be Tested?” — suggests a whopping 80% of Americans are insulin resistant, and that’s true even if your fasting glucose is normal.4,5
The good news is that insulin resistance is one of the easiest health problems to correct. Below I review eight of my top tips for optimizing and maintaining a healthy blood sugar level.
Tip No. 1 — Proper Meal Timing
Intermittent fasting or compression of your eating window is a powerful approach that facilitates weight loss and helps reduce your risk of chronic diseases like Type 2 diabetes.
In his book “Circadian Code: Lose Weight, Supercharge Your Energy and Sleep Well Every Night,” Satchidananda Panda, Ph.D., cites research showing that 90 percent of people eat across a span of 12 hours a day, and many across even longer timespans, which is a clear prescription for metabolic disaster.
Intermittent fasting, i.e., the cycling of feast (feeding) and famine (fasting) mimics the eating habits of our ancestors and restores your body to a more natural state that allows a whole host of metabolic benefits to occur.6
With regard to insulin resistance, research shows intermittent fasting promotes insulin sensitivity and improves blood sugar management by increasing insulin-mediated glucose uptake rates.7
While there are a number of different intermittent fasting protocols, my preference is fasting daily for 18 hours and eating all meals within a six-hour window. If you’re new to the concept of intermittent fasting, consider starting by skipping breakfast and have your lunch and dinner within a six-hour timeframe, say 11 AM and 5 PM, making sure you stop eating three hours before going to bed.
The latter is important, as it helps protect your mitochondrial function. Recent research8,9 shows men who are at risk of Type 2 diabetes can improve their glucose control, thereby lowering that risk, simply by eating all their meals within a nine-hour timeframe — even if they do not implement any other dietary changes.
Research10,11 has also shown men who eat supper at least two hours before bedtime have a 26% lower risk of prostate cancer, and women have a 16% lower risk of breast cancer than those who eat dinner closer to bedtime. For more details on why late-night eating is so detrimental, see “Eating Early Dinner Aids Weight Loss and Lowers Cancer Risk.”
When you do eat, focus on healthy protein in moderate amounts and minimize net carbs like pasta and bread, exchanging them for healthy fats like butter, eggs, avocado, coconut oil, olive oil and raw nuts. This will help shift you into fat burning mode.
On a related side note, when eating, relax and take your time! Research shows rushed eating, which typically occurs when you’re stressed, has a significant impact on your blood sugar level. When you become stressed your body also secretes cortisol and glucagon, both of which affect your blood sugar levels as well.12 You can learn more about this in “How Stress Can Affect Your Blood Sugar Level.”

Tip No. 2 — Monitor Your Blood Sugar Level
As mentioned, while prediabetes13 is clinically defined as having a fasting blood sugar level between 100 and 125 mg/dl, I strongly believe any blood sugar over 90 mg/dl puts you in the danger zone for insulin resistance. Your blood sugar is measured through a glucose test, of which there are four types:
- Fasting plasma glucose test — When you fast overnight and take your blood sample in the morning
- Oral glucose tolerance test — Similar to the fasting blood sugar test, overnight fasting is required for this, and the person’s fasting blood sugar level is measured. Afterward, a sugary liquid is provided and the levels are then tested for the next two hours
- Hemoglobin A1C test — This test checks the percentage of blood sugar attached to the hemoglobin and will indicate your average blood sugar level for the past two to three months
- Random plasma glucose test — This makes use of a blood sample that is taken at a random time
You could also do 24-hour continuous glucose monitoring, which I’ve done in the past, although it’s pricey and probably not necessary for most people.
At the time, I used a Dexcom monitor, which involves inserting a sensor beneath your skin for a week, which takes continuous glucose readings every few minutes. It really helped me fine-tune and evaluate how different foods impacted my glucose levels, and helped me understand the importance of feast-famine cycling.
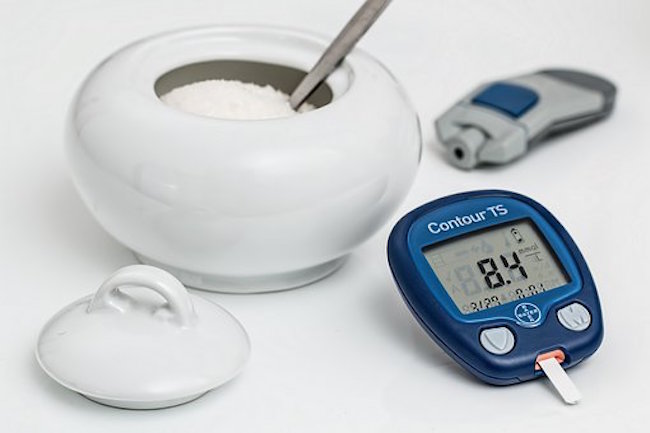
All of that said, for most people, a simple at-home glucose test,14 where you prick your finger and deposit a drop of blood onto a glucose testing strip, will do the job. Ideally, test yourself two to three times a day: first thing in the morning, before your first meal, and a couple of hours after your last meal.
Your blood glucose levels will vary throughout the day. According to conventional recommendations, if you are healthy and do not have diabetes, your fasting blood glucose upon waking should be below 100 mg/dL. I recommend aiming for a fasting (when you wake up) level below 90 mg/dL.
Before meal time, your glucose level should read between 70 to 99 mg/dL. After meals — or what’s called “postprandial” and is usually taken two hours after eating — the level should be below 140 mg/dL.
There are two measurements used for blood sugar levels. In the U.S., the measurement is in milligrams of glucose per deciliter of blood (mg/dL). In the U.K. and Canada, the measurement for blood sugar is in millimoles/liter (mmol/L). To convert to mg/dL, multiply the amount by 18. For example, if a person in the U.K. says that their blood glucose result is 7 mmol/L, in the U.S. it’s read as 126 mg/dL.
Tip No. 3 — Monitor Your Blood Ketones
Another valuable test is the blood ketone test, which will tell you whether you’re in nutritional ketosis or not. I recommend starting your intermittent fasting routine and monitoring your blood ketones as you go along. The KetoCoachX monitor15 is currently one of the best and least expensive ketone monitors on the market.
Continue Reading / Mercola>>>